Clinical context
Echinococcosis
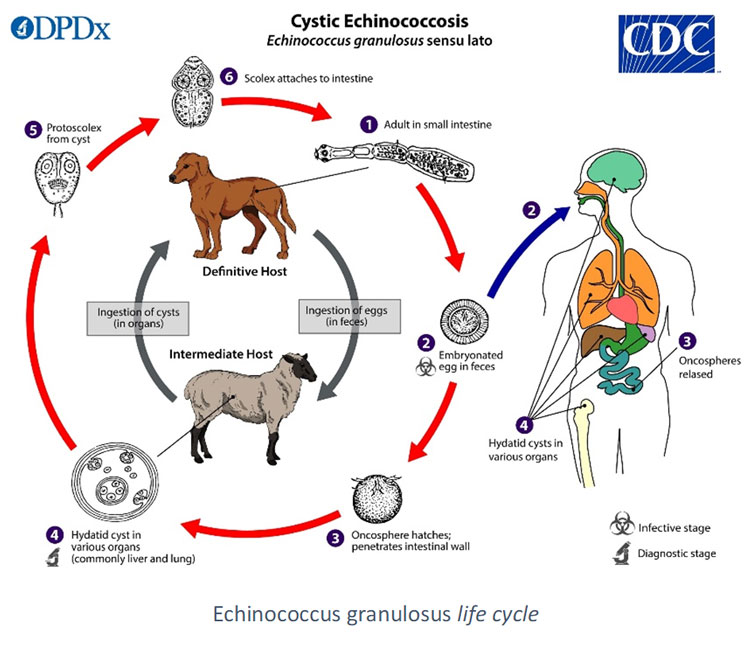
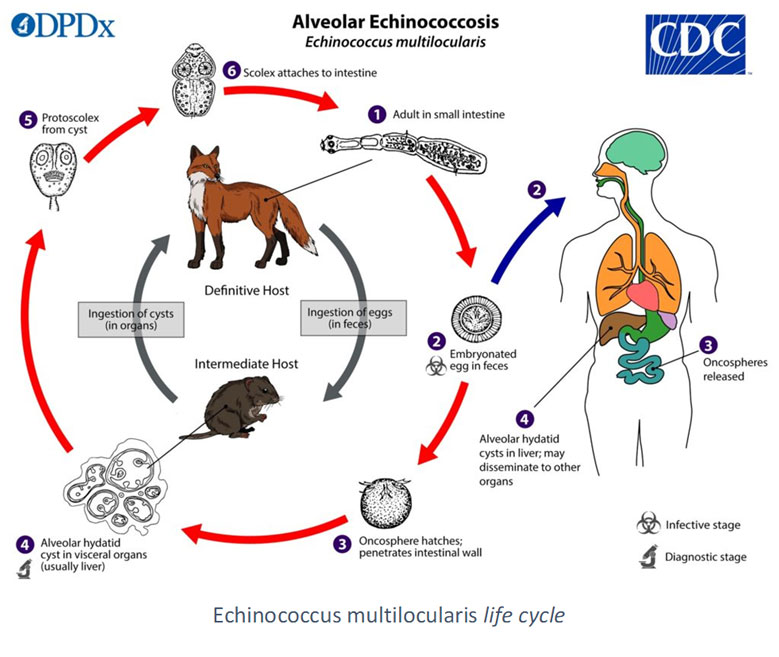
Echinococcosis are parasitic zoonoses due to tapeworm larvae belonging to the Echinococcus genus, parasiting the intestine of wild and domestic canines. Beside canines (mostly dogs and foxes for E. multilocularis), cats are sometimes found as accidental definitive hosts. Humans, as the other omnivorous and herbivore intermediate hosts, gets infected by ingestion of eggs, eliminated in nature or present on the fur of definitive host. Transmission in humans usually occur by ingestion of unsufficiently rinsed fruits or vegetables contaminated by feces of the definitive host. The egg releases a larva which migrates through blood or lymphatic stream before being stopped mostly by the liver, but also other organs such as lungs. Larvae develop in cysts, which can either grow progressively larger (E. granulosus) or form buds, which upon detachment form secondary cysts (E. multilocularis) (Woolsey & Miller, 2021).
Four species are responsible of human chronic and severe diseases, infecting between 2 and 3 million people (Cerda et al., 2018). There is a clinical latency of several years between infection and symptoms onset.
- E. granulosus, present worldwide, is responsible of cystic echinococcosis, and is frequent in places where veterinary surveillance is lacking. It is the cause of important economic losses, as the infection also reaches livestock.
- E. multilocularis, that circulates in the northern hemisphere, is the agent of alveolar echinococcosis.
- E. vogeli and E. oligarthus are responsible of polycystic echinococcosis in Latin America, where they are considered as emergent parasitoses.
- Besides, coinfections with both E. multilocularis and E. granulosus have been encountered in central Europe, Russia and China (McManus et al., 2003).
The infection is often of poor prognosis, lethal if untreated. In humans, Echinococcus spp. multiply and reorganize to form larvae with complex structures. The endogenous/exogenous development as well as the intra-visceral organization differ from one species to another (Thompson, 2017).
In 70% of cases E. granulosus embryos are located in the liver, but can also be found in the lungs or in other organs (heart, bones, spleen or central nervous system). Its cells bud and form vesicles containing protoscolexes and a clear liquid. At least for the hepatic locations, the larva develops in a hydatid cyst. Clinical manifestations differ according to the location, size and number of cysts. They are directly linked to the progressive invasion of the organs or their compression. Accidental rupture of a cyst may result in immediate hypersensitivity manifestations, triggered by the cystic liquid, and in the formation of secondary cysts from protoscolex newly externalized (Higuita et al., 2016).
- E. multilocularis, the most pathogenic of the Echinococcus species, mainly invades the liver. The proliferation of its cells is exogenous. The larva progressively infects the organ and causes an intense granulomatous reaction followed by a diffuse fibrosis. As a result, parasitic cells can also create secondary cysts. Clinically, alveolar echinococcosis mimicking hepatocarcinoma (Brunetti et al., 2010).
- E. vogeli and E. oligarthus multiply mainly endogenously, but sometimes exogenously. They form liquid vesicles that remain linked to the index cyst, giving a grapefruit aspect. The hepatic location is more frequent than isolated pulmonary, cardiac, mesenteric, ocular locations or multi-visceral forms. The prognosis of polycystic echinococcosis is close to the one of alveolar echinococcosis. (D’Alessandro, 1997).
Direct parasitological examination of echinococcosis is very invasive and therefore rarely possible. Puncture of a cyst for diagnosis is contraindicated because of the high risk of anaphylactic incident due to the rupture of the cyst, but may be done in a curative surgical context. The diagnosis, guided by biological abnormalities (especially for alveolar echinococcosis) and morphological abnormalities (detected with imagery, mainly by ultrasound), relies on serology. Serodiagnosis is essential for the rapid medical support of patients.
Treatment is both medical and surgical: albendazole for several years if not for life, and whenever possible, surgery. This surgery depends on the size, location and number of lesions. It consists in removing the cyst content by PAIR technique (Puncture, Aspiration of the parasitic mass, Injection of salt serum and Re-aspiration), or removing the infected part of the organ (partial hepatectomy for instance).
Amongst classical serology techniques, the most frequently used is ELISA. Frequent cross-reactions (with other helminthiases and during other pathologies, in particular other hepatic diseases) observed with non-purified antigens lead to the use of synthetic antigens (synthetic peptides, recombinant antigens). These ELISAs may lack of sensitivity (Wen et al., 2019). Due to these limitations, a positive or equivocal serological diagnosis must be verified by Western Blot to confirm the diagnosis.
SCIENTIFIC REFERENCES
- Atanasov G, Benckert C, Thelen A, Tappe D, Frosch M, Teichmann D, et al. Alveolar echinococcosis-spreading disease challenging clinicians: A case report and literature review. World J Gastroenterol. 2013 Jul 14;19(26):4257–61.
- Auer H. [Relevance of parasitological examinations for the clinical course, epidemiology and prevention of alveolar echinococcosis – experiences of more than two decades in Austria]. Wien Klin Wochenschr. 2006;118(19-20 Suppl 3):18–26.
- Bart J-M, Piarroux M, Sako Y, Grenouillet F, Bresson-Hadni S, Piarroux R et al. Comparison of several commercial serologic kits and Em18 serology for detection of human alveolar echinococcosis. Diagn microbiol and infect dis 2007 59(1):93–95
- Brunetti E, Kern P, Vuitton DA, Writing Panel for the WHO-IWGE. Expert consensus for the diagnosis and treatment of cystic and alveolar echinococcosis in humans. Acta Trop. 2010 Apr;114(1):1–16.
- Furuya K, Kawanaka M, Yamano K, Sato N, Honma H. [Laboratory evaluation of commercial immunoblot assay kit for serodiagnosis of Echinococcus infections using sera from patients with alveolar hydatidosis in Hokkaido]. Kansenshogaku Zasshi. 2004 Apr;78(4):320–6.
- Lassen B, Janson M, Viltrop A, Neare K, Hütt P, Golovljova I et al. Serological Evidence of Exposure to Globally Relevant Zoonotic Parasites in the Estonian Population. PLoS One 2016 Oct 10;11(10):e0164142
- Liance M, Janin V, Bresson-Hadni S, Vuitton DA, Houin R, Piarroux R. Immunodiagnosis of Echinococcus infections: confirmatory testing and species differentiation by a new commercial Western Blot. J Clin Microbiol. 2000 Oct;38(10):3718–21.
- Logar J, Soba B, Kotar T. Serological evidence for human cystic echinococcosis in Slovenia. BMC infect dis, 2008; 8:63
- Logar J, Soba B, Lejko-Zupanc T, Kotar T. Human alveolar echinococcosis in Slovenia. Clin Microbiol Infect. 2007 May;13(5):544–6.
- Makni F, Hachicha L, Mseddi F, Hammami H, Cheikhrouhou F, Sellami H, et al. [Contribution of Western blotting to the diagnosis of hydatidosis]. Bull Soc Pathol Exot. 2007 Aug;100(3):171–3.
- Otranto D, Eberhard ML. Zoonotic helminths affecting the human eye. Parasit Vectors. 2011 Mar 23;4:41.
- Reiter-Owona I, Grüner B, Frosch M, Hoerauf A, Kern P, Tappe D. Serological confirmatory testing of alveolar and cystic echinococcosis in clinical practice: results of a comparative study with commercialized and in-house assays. Clin Lab. 2009;55(1–2):41–8.
- Rinaldi F, Brunetti E, Neumayr A, Maestri M, Goblirsch S, Tamarozzi F. Cystic echinococcosis of the liver: A primer for hepatologists. World J Hepatol. 2014 May 27;6(5):293–305.
- Tappe D, Grüner B, Kern P, Frosch M. Evaluation of a Commercial Echinococcus Western Blot Assay for Serological Follow-Up of Patients with Alveolar Echinococcosis. Clin Vaccine Immunol. 2008 Nov;15(11):1633–7.
- Vicidomini S, Cancrini G, Gabrielli S, Naspetti R, Bartoloni A. Muscular cystic hydatidosis: case report. BMC infect dis 2007 30 (7):23
- Yamano K, Yagi K, Furuya K, Sawada Y, Honma H, Sato N. Active alveolar hydatidosis with sero-negativity for antibody to the 18 kDa antigen. Jpn J Infect Dis. 2005 Apr;58(2):122–4.
- Zait H, Achir I, Guerchani MK, Hamrioui B. [Epidemiological profile of 290 cases of human cystic echinococcosis diagnosed in the Mustapha University Hospital (Algiers) from 2006 to 2011]. Pathol Biol. 2013 Oct;61(5):193–8.
- Zait H, Hamrioui B. Human cystic echinococcosis: Serological diagnosis by indirect hemagglutination test, enzyme-linked immunosorbent assay, immunoelectrophoresis, and immunoblotting in surgically confirmed patients versus cases diagnosed by imaging techniques. Méd. Mal. Inf. 2019 Nov 11.
ECHINOCOCCUS Western Blot IgG TEST
Specificity and sensitivity of the immunoblot lead to propose this technique as confirmation of screening tests, and as a differentiating assay for the two main human echinococcosis : alveolar and cystic echinococcosis.
The Haute Autorité de Santé (HAS) in France as well as the American Center for Disease Control (CDC) recommend the immunoblot for the confirmation of serodiagnoses (Argumentaire HAS, 2017, DDPx Echinococcus, 2019).
In order to meet this demand, we developed a reliable test based on the Western Blot technique. Associated with highly sensitive natural antigens, the ECHINOCOCCUS Western Blot IgG test is a robust confirmation technique of classical screening tests (Liance et al., 2000, Yamano et al., 2004, Bart et al., 2007, Vola et al., 2019). It allows the differential diagnosis between E. granulosus and E. multilocularis infections.
Several studies reported its pertinence in the follow-up of patients with alveolar echinococcosis (Tappe et al., 2008), and post-surgery follow-up of cystic echinococcosis (Makni et al., 2007). It also seems to be more sensitive than other commercial kits (Deininger & Wellinghausen, 2019, Tamarozzi et al., 2019).
Our products
Order
To order a product, please send us an email to our address Order with the description of the product. We ship worldwide.